October 18, 2019
Clinical Integration Report on Using the Armeo®Spring in a Parallel Setting for Neurological Injury Rehabilitation
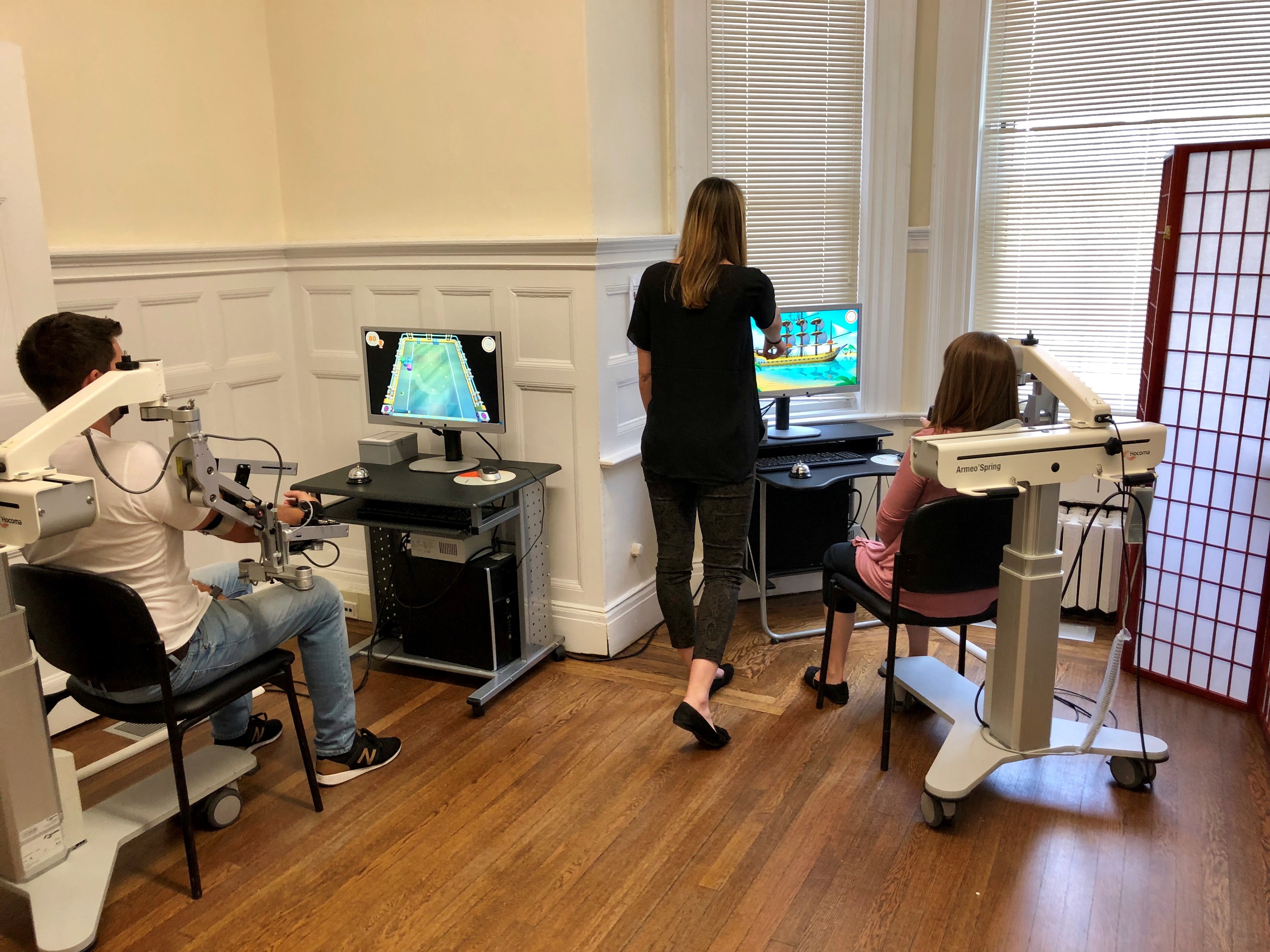
Burke Neurological Institute, White Plains, USA
We have been working with the ArmeoSpring since January 2017 in which we had utilized the devices for a clinical research trial to look at effects of staff to participant ratio (1:1 vs. 1:2) and treatment dosage (30 min. vs. 60 min) in an outpatient research setting. Here we would like to share our experience with using the devices in the 1:2 staffing ratio.
Patient Group
Our participants had unilateral or bilateral upper extremity paresis as a result of a neurological injury, which included Individuals with stroke, traumatic brain injury, brachial plexus injury, and spinal cord injury. All participants were in the chronic stage (>6 months post injury).
All participants had medical clearance from their doctor in order to participate in active therapies, and were able to follow 1-2 step commands and tolerate repetitious movement.
There were no other restrictions that prevented use of the device (fixed joint contractures, severe spasticity, etc.).
Duration and Frequency of Armeo®Spring Sessions
Participants came three times a week for 6 weeks, totaling 18 sessions. Each session was scheduled for 30 or 60 minutes of active therapy time.
Each participant had an individualized training plan based on their initial active movement. Exercises were selected by a certified therapist based on participant’s initial evaluation. Active movement in at least 1 DOF of a joint was required for exercises involving that particular joint to be included in their training.
Once the exercises were selected, the type and order of exercises were kept consistent throughout the study. Exercise length was between 2-10 minutes each. The therapist could alter game difficulty level (1-3) to match the participant’s current skill level. All participants started at level 1; if an individual received a 5/5-star rating on an exercise for 2 consecutive visits or the participant reported the exercise being “too easy”, the level was advanced to the next.
Patient Evaluation
We administered clinical and robotic evaluations at admission and again after 18 treatment sessions. Clinical assessments included: Upper Extremity Fugl-Meyer, Box and Blocks, grip strength, and quality of life questionnaires.
1:2 Staffing Ratio Feasibility
The ArmeoSpring allows for semi-autonomous therapy with supervision from trained staff, making it feasible for two participants to be treated at the same time by one staff member.
To allow time for set up (5 minutes), participants were asked to arrive 5 minutes prior to their session time. This way both participants were able to be set up prior to their start time. Participants were seated so that they could see the other participant in their peripheral vision, but they could not see their screen in order to decrease distraction.
In our experience, it was best to stagger the start times of the exercises for each participant by at least 30 seconds. This way the two participants were not transitioning to new exercises at the same time, due to the fact that the therapist would often have to lock or unlock joints in between exercises. However, staggered timing may be disrupted if a technical issue occurs and the exercise needs to be paused while solving it.
Overall, the 1:2 staffing ratio did not alter the participant’s time on task when compared to the 1:1 group, showing that it is feasible for one therapist to see two participants at the same time on the ArmeoSpring. Staff reported ease of supervising two participants at once during this type of training.
Participants in the 1:2 staffing ratio group showed greater impairment reduction after 18 sessions than individuals in the 1:1 group. For the Upper Extremity Fugl-Meyer the Pre – Post difference was 4.45 ± 3.00 points for individuals in the 1:2 staffing ratio group and 2.75 ± 2.66 points for individuals in the 1:1 group.
Participants were also asked to complete a questionnaire at the end of their 18 sessions which asked questions about their experience based on a 5-point Likert scale. The majority of participants in the 1:2 treatment group reported that they were not distracted by the other participant, they felt like they were receiving enough individual attention, and they enjoyed the experience.
Reasons to Include the Armeo®Spring as Part of the Therapy Program
The ArmeoSpring provides intensive upper extremity training in a 3D workspace. The ability to lock and unlock joints allows for a wide variety of impairment levels to use the device and still find it challenging.
Even though the device only offers spring assistance, we were able to have participants with severe upper extremity impairment successfully utilize the device (Fugl-Meyer score ≥8). We found it beneficial to use a strap attached to the chair to limit trunk compensation for lower level participants.
Participants frequently reported that the exercises were engaging and the feedback from the scoring allowed them to be competitive with themselves.
To facilitate a 1:2 therapist to patient ratio in a clinical setting, we would recommend a staggered arrival of patients.
Organization: Responsible Therapy Team
Our team consists of trained clinical research staff and certified occupational therapists.
The certified therapists were responsible for conducting evaluations, initial set-up, selecting therapy programs, and adjusting the progression as needed. The trained staff members received distant supervision from the therapists and were trained to set up, adjust the equipment (locking and unlocking of joints) for different movements based on the exercise, troubleshoot any technical difficulties, and removal of the patient from the device.
About Us
Burke Neurological Institute is a nonprofit leading scientific research institute devoted to advancing the study of neurological diseases and injuries, pioneering novel rehabilitation therapies and developing innovative clinical programs and clinics.
At Burke Neurological Institute our goals is to combine the most rigorous, contemporary, brain science with heartfelt compassionate care to innovate and develop novel cures for stable disability in those afflicted with neurological conditions such as stroke, traumatic brain injury, or spinal cord injury.
This clinical experience report is meant to serve as an example of how the ArmeoSpring is integrated into one particular rehabilitation centre. It is not necessarily a standard recommendation from Hocoma.